AI Data Governance in Healthcare: How Poor Data Quality Is Affecting Patient Outcomes in Healthcare
As data sharing expands, strong data governance is no longer optional. In this article, we explore what data governance in healthcare means, how poor governance impacts patient safety, why delaying governance is risky, and real-world use cases of AI-driven data governance in healthcare.

Fix Inaccurate Patient Records Using AI-Driven Data Stewardship to Improve Safety and Clinical Outcomes Consistently

Understanding AI Data Governance in Healthcare and Its Impact on Patient Outcomes
Any highly regulated sector requires strong governance, but AI data governance in healthcare is uniquely critical due to its direct impact on patient safety, compliance, and clinical outcomes. Robust governance is necessary rather than optional because even small data inaccuracies might result in major health hazards. This is due to the fact that it collects and utilizes vast amounts of personal data to make informed decisions about patient care. In addition to causing noncompliance and audit problems, incomplete data can also cause injury to actual persons. For instance:
- Inaccurate information can potentially result in further insurance coverage delays.
- Healthcare organizations must abide by data privacy regulations, including GDPR and HIPAA. In addition to putting patients and practitioners at risk when data breaches occur, breaking these regulations can be costly.
- Medical records are frequently used by healthcare professionals to diagnose patients and create treatment strategies. Serious repercussions can result from inaccuracies in these medical data, including misdiagnoses, drug errors, or delayed care.
Healthcare organizations can use predictive analytics to find patterns, trends, and future health problems in patients. Most electronic health record systems have predictive analytics capabilities, which are noteworthy. The precision of the data used determines how accurate these analytics can be.
How Poor Data Governance in Healthcare Affects Patient Safety
According to a Jama Network survey, 20% of patients found errors in their medical records, and 40% thought these errors were substantial. Errors occurred in diagnosis, medical history, prescriptions, physical examination, test results, and documentation related to the incorrect patient. These errors do not occur due to clinical negligence. Their occurrence is due to the lack of direct communication between Epic and Cerner, necessitating costly interface development, as the pharmacy system was deployed by a supplier rather than the laboratory system.
A patient arrives at the emergency department. When the attending physician opens the patient’s chart, they discover a list of medications from 2023, allergy fields that read “NKDA” despite the patient’s insistence that they had notified someone about a penicillin response last year, and test results that don’t reflect the bloodwork completed two weeks ago at an urgent care facility. The doctor chooses a course of treatment since the patient is uncomfortable, and waiting for a detailed chart is not an option.
The repercussions go beyond specific patient interactions:
- Redundant medication prescriptions arise when a single patient is enrolled under two distinct Medical Record Numbers (MRNs), leading to the oversight of their existing warfarin treatment.
- An error in patient identification caused lab results to sit unreviewed for three days. When the issue was finally detected, the patient had already left, and the abnormal findings could not be communicated due to incorrect contact details.
- Instead of doing the chart checks for which they were employed, HIM employees spend half of their day reconciling duplicate records.
How to Implement AI Data Governance in Healthcare
The initial stage of executing AI data governance in healthcare is the establishment of a robust framework. This entails establishing policies, standards, and procedures for data management. Establish roles and duties to ensure that all individuals are aware of their contributions to upholding data integrity.
A thorough framework must encompass:
- Data Stewardship: Designate individuals or teams to monitor data quality and ensure compliance.
- Policies & Procedures: Formulate comprehensive policies for data access, exchange, and protection.
- Data Governance Council: To devise and enforce data governance policies, establish a council.
Data Quality and Maturity: How Accurate and Trustworthy Is Your Data?
One cannot govern something one cannot quantify. Accuracy, completeness, consistency, timeliness, and validity are used to gauge data quality.
Data Maturity Measuring
How “mature” is your business in terms of data? Most businesses take the following steps:
- Defined: Data management for healthcare is governed by a company-wide policy.
- Managed: KPIs and dashboards track data quality.
Data Confidentiality
Confidentiality in healthcare is a human right, not only a feature. Data management entails putting “Privacy by Design” into practice, which comprises:
- Anonymization: Eliminating personal information to allow researchers to examine diseases without identifying the sufferers.
- Access Control: Ensuring that important psychiatric or oncological records are only accessible to the authorized physician.
- Audit Trails: Identifying precisely who accessed what information and when.
For Leaders Who Feel Governance Can Wait Until AI is “More Mature,” What Usually Happens When They Delay?
When healthcare leaders delay AI data governance, issues emerge quickly, fragmented EHR data, inconsistent coding (ICD-10, SNOMED), and poor data lineage lead to biased models and unsafe clinical recommendations.
Privacy gaps expose PHI, increasing HIPAA violation risks. Without early controls, model drift goes undetected, degrading accuracy in predicting readmissions or sepsis. Regulatory audits become reactive and costly, while clinician trust declines due to unreliable outputs.
Over time, fixing these gaps requires rework across data pipelines, training datasets, and compliance frameworks. Delayed governance doesn’t slow risk; it amplifies it, directly impacting patient safety, outcomes, and organizational credibility.
Why AI Data Governance in Healthcare is Important: Key Benefits
AI data governance framework healthcare ensures accurate, secure, and consistent data across systems. It improves patient safety, supports regulatory compliance, reduces errors, and enables reliable analytics and AI. Strong governance helps healthcare organizations make better decisions and deliver higher-quality care.
1. Enabling Care Coordination & Interoperability
A major challenge in healthcare is the integration of systems. As a result, interoperability has become crucial due to the growing adoption of electronic health records (EHRs) by hospitals. Data governance enables this by:
- Implementing standards like FHIR to provide consistency across systems.
- Utilizing tools such as knowledge graphs to establish connections between pertinent data points.
In this way, hospitals and clinics can operate with a consistent, precise understanding of a patient’s health.
2. Supporting Healthcare Research & Innovation
Healthcare innovation depends on data for the development of new medicines and the training of AI systems. Nonetheless, governance is essential for the safe and ethical utilization of that data. It ensures that:
- The research data is correct and clearly labeled.
- When necessary, patient information is de-identified.
For instance, AI data governance in healthcare ensures that privacy regulations are adhered to and that the data is suitable for use when hospitals share data with researchers, ensuring that innovation advances on a solid foundation.
3. Improving Patient Outcomes through Data Quality
Patients are at risk when data is disorganized or out-of-date because inaccurate diagnoses or prescriptions might result from bad records. This is a significant factor in the over 250,000 deaths that occur in the United States each year due to medical errors. Efficient governance ensures that:
- Patient records are accurate, complete, and consistently maintained.
- Errors are identified and resolved at an early stage to prevent downstream impact.
4. Ensuring Regulatory Compliance
One of the sectors with the strictest regulations is healthcare. Strict guidelines for the handling of patient data are established by laws such as the CCPA, GDPR, and HIPAA. Cyberattacks exposed the health information of roughly 167 million Americans in 2023 alone. Such a violation can result in significant penalties and a decline in patient confidence.
In 2023, the U.S. Office for Civil Rights imposed fines totaling over $4 million.
Use AI in data governance to avoid such high fines. It maintains compliance for healthcare businesses by:
- Limiting data access.
- Controlling data deletion, sharing, and storage.
Accelerate Clinical Decision Support with Explainable AI Models Backed by Transparent and Compliant Data Governance
How Generative AI Governance Powers Real Healthcare Use Cases Safely at Scale
To enhance care, boost productivity, and ensure adherence to local, state, and federal laws, hospitals, clinics, and government organizations are putting AI governance into practice. Let’s examine some of the most popular applications for Generative AI data governance in healthcare.
 1. Digital Twins to Speed Up Clinical Research
1. Digital Twins to Speed Up Clinical Research
AI-powered digital patient simulations help clinicians test treatment pathways, evaluate drug responses, and design safer clinical trials using real-world patient data such as EHRs, lab results, and imaging records.
Robust AI governance ensures that these models adhere to medical rules, safeguard sensitive health information such as PHI, and reduce bias in outcomes among varied patient populations. It also improves transparency in clinical decision support systems, auditability of AI models, and trust among physicians, regulators, and researchers, ensuring that AI-driven insights lead to safe, ethical, and effective patient care.
2. Clinical Guidance Systems & Customized Care Strategies
Medical professionals can receive recommendations from AI based on its evaluation of patient information, scientific publications, and healthcare protocols. AI oversight reduces the possibility of errors by ensuring that these insights are accurate, unbiased, and comprehensible.
AI data management for healthcare uses personal medical records, genetic profiles, and current health data to modify treatment strategies. It promotes conformity to regulatory requirements, protects patient privacy, and clarifies clinical decisions.
3. Forecasting Algorithms to Anticipate Patient Health Outcomes
Artificial intelligence in healthcare can predict disease progression, 30‑day readmissions, sepsis risk, ICU transfer, and medication response using EHR data, lab results, imaging, and genomics. Strong governance ensures clean data, bias checks, audit trails, and HIPAA compliance. Standardized coding (ICD‑10, SNOMED, LOINC) improves accuracy.
Clinician oversight, model validation, and explainable outputs build trust. Secure deployment, role‑based access, and continuous monitoring prevent errors, data leaks, and unsafe recommendations, enabling fair, reliable, and clinically useful AI insights.
4. Enable Population Health & Analytics
Accurate patient cohorts are essential to population health initiatives. Your outreach lists and prevalence estimations are incorrect if your system indicates that you have 10,000 diabetes patients, but 1,500 of those are duplicated. Analytics and reporting gain reliability when founded on credible master data. When your data quality measurements or financial dashboards rely on disorganized, redundant, or inconsistent data, the findings cannot be trusted.
Capacity planning, forecasting, and budgeting rely on comprehending the demographics of your patients, their origins, and the services they require. Dispersed data compromises all of that.
5. Patient Identity Resolution
The most prominent application of AI in master data management healthcare is patient identity resolution. This is often administered via a Master Patient Index (MPI) or an Enterprise Master Patient Index (EMPI). Upon a patient’s arrival at the emergency room, the system must ascertain whether the provided name and birthdate correspond to an existing database entry or indicate a new patient. Erroneous input results in the creation of a duplicate record. Excessive caution may result in the conflation of two distinct individuals, which is more detrimental.
Effective master data management healthcare minimizes duplicate and overlapping records while avoiding erroneous matches. It accomplishes this via probabilistic or deterministic matching algorithms that evaluate similarity across various data points. An exact correspondence in name, date of birth, and Social Security number is unequivocal. A partial match using a phonetically analogous name with a transposed birthday is more challenging.
Minimize Regulatory Risks by Embedding Privacy by Design Principles into Healthcare Data Lifecycle Management Practices
How a Data Governance Team Supports Successful Data Management for Healthcare
Given the substantial number and essential nature of health data, healthcare data quality management necessitates a collaborative approach. Ensuring the security, accessibility, compliance, and interoperability of clinical, financial, and commercial data necessitates the involvement of personnel throughout the healthcare organization. Facilitating this initiative is crucial.
A healthcare data governance team can be an asset by collaborating across functions to build robust strategies, policies, and plans that effectively serve the corporation. Governance teams encompass various organizational functions, including compliance, legal, business operations, and technical teams. Members of the senior leadership, including the C-suite and senior management stakeholders, participate in a Data Governance Council that establishes overarching direction and policies.
At What Stage of the AI Development Should Healthcare Organizations Start Thinking About AI Governance?
Healthcare organizations should start thinking about AI governance at the earliest stages of AI development, right from problem definition and data selection. Waiting until deployment increases risks around compliance, bias, and patient safety. Early governance ensures AI systems are clinically reliable and ethically sound.
- During data collection and preparation, enforce standards like FHIR, ICD-10, and LOINC to ensure consistency and reduce bias in training datasets.
- At the model development stage, implement validation protocols, explainability requirements, and audit trails to maintain transparency.
- In testing and deployment, apply role-based access, privacy controls, and HIPAA-aligned safeguards to protect sensitive patient data.
- During post-deployment monitoring, continuously track model drift, performance gaps, and real-world clinical impact.
By embedding governance from the start, healthcare organizations can build scalable, compliant, and trust-driven AI systems that improve patient outcomes while minimizing risk.
Core Pillars of a Strong Data Governance Framework Healthcare
A comprehensive data governance strategy in healthcare is founded on several essential components, each crucial for maintaining the integrity and effectiveness of the data management process.
- Regulatory Compliance: Strategies for data governance must comply with legal and regulatory obligations. This entails abiding by regulations in the healthcare industry, such as HIPAA in the United States, which requires the security of health information and the preservation of patient privacy.
- Policy Development: It is crucial to develop thorough data governance policies. These guidelines ought to address data management, storage, sharing, and security. They must be unambiguous, enforceable, and updated frequently to consider modifications to the regulatory and healthcare environments.
- Data Quality: Ensuring data quality is essential to any data governance plan. This includes the reliability, correctness, and completeness of medical data. For precise clinical decision-making and efficient healthcare delivery, great data quality is essential.
- Organizational Goals Alignment: Your healthcare organization’s overarching goals should be supported by the data governance plan. The approach should support these objectives through efficient data management, whether they are improving patient outcomes, expanding research capacities, or boosting operational effectiveness.
Future Trends of AI Data Governance in Healthcare for 2026
As AI becomes more integrated into clinical and operational operations this year, the change is already apparent. FHIR connections and real-time exchanges make data flows more integrated, and regulations keep up with practical use cases. To safeguard patient data while fostering innovation, healthcare data governance must adjust to these developments. These developments are already influencing 2026’s priorities.
- Unified Governance for Real-Time Data and Seamless Interoperability: Payers demand near-real-time evaluations of readmissions and quality measures. This necessitates governance that manages continual quality checks and event-driven feeds without the need for human intervention. In hybrid configurations, data governance systems develop to automate compliance and lineage tracking. The results are smoother interactions, fewer rejections, and more robust population health initiatives.
- Enhanced Controls for AI Model Training and Privacy Protection: The use of protected health data in AI models is coming under increased scrutiny. Rules increasingly call for audit trails for training procedures, explicit consent procedures, and synthetic data substitutes. Stricter protections are applied to patient data privacy, particularly in multi-state or multinational settings. By taking these precautions, you can ethically promote AI-driven insights in care coordination and diagnostics while avoiding enforcement actions.
- AI Governance Moves from Optional to Essential: AI systems currently manage documentation, risk assessment, and administrative functions extensively across numerous enterprises. In the absence of devoted oversight, the issues associated with prejudice, transparency, and the abuse of PHI escalate rapidly. Anticipate an increase in health systems establishing AI governance committees, developing approved tool inventories, and formulating procedures for model training data and output verification. This transition ensures that AI outputs are defensible under HIPAA and facilitates assured clinical use.
These trends demonstrate how governance is becoming a strategic function rather than a compliance chore. Concentrate on the ones that best fit your present interoperability gaps or AI initiatives. By addressing them early on, you put your business in a position to effectively manage rapid change.
How NextGen Invent Enables Scalable and Efficient AI Data Governance in Healthcare
In a digital-first care ecosystem, AI-driven systems rely on EHRs, imaging, genomics, and real-time monitoring data to predict outcomes and guide treatment. Without structured AI data governance services, risks such as model bias, PHI exposure, and regulatory violations increase, affecting patient safety and trust.
- Standardized data models using FHIR, SNOMED, and LOINC ensure consistency across systems.
- Continuous model validation and audit trails improve transparency and clinical accountability.
With digital health software development services, NextGen Invent strengthens governance through role-based access, consent management, and secure pipelines for training and deployment. This enables explainable AI, reduces data silos, and supports HIPAA and global compliance.
- Clinicians access accurate, real-time insights for safer decisions.
- Administrators maintain regulatory readiness without delays.
Scalable AI governance transforms healthcare data into trusted intelligence, driving innovation, improving outcomes, and ensuring the secure, ethical adoption of AI for future-ready systems.
Frequently Asked Questions About AI Data Governance in Healthcare
Related Blogs

Multimodal AI Use Cases: How Multimodal Models Work and How Enterprises Are Scaling Generative AI
The next wave of competitive advantage will not come from better prompts alone, but from multimodal AI use cases that combine text, images, audio, video, and structured data to mirror how the real world works.
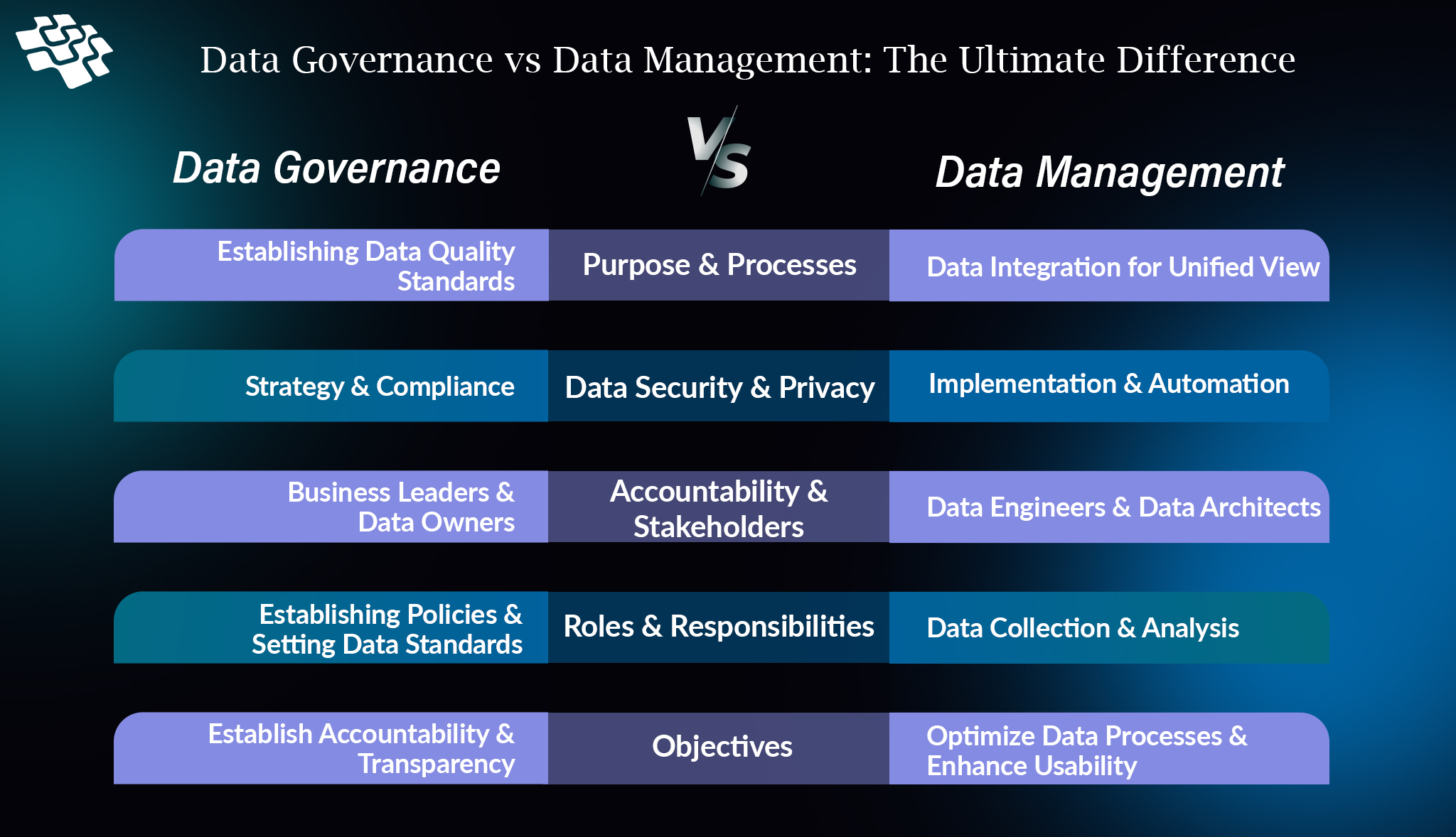
Data Governance vs Data Management: The Ultimate Comparison
Organizational structures, data owners, rules, procedures, business language, and metrics for the entire lifecycle of data are all defined by data governance. Data management is the technical execution of data governance.
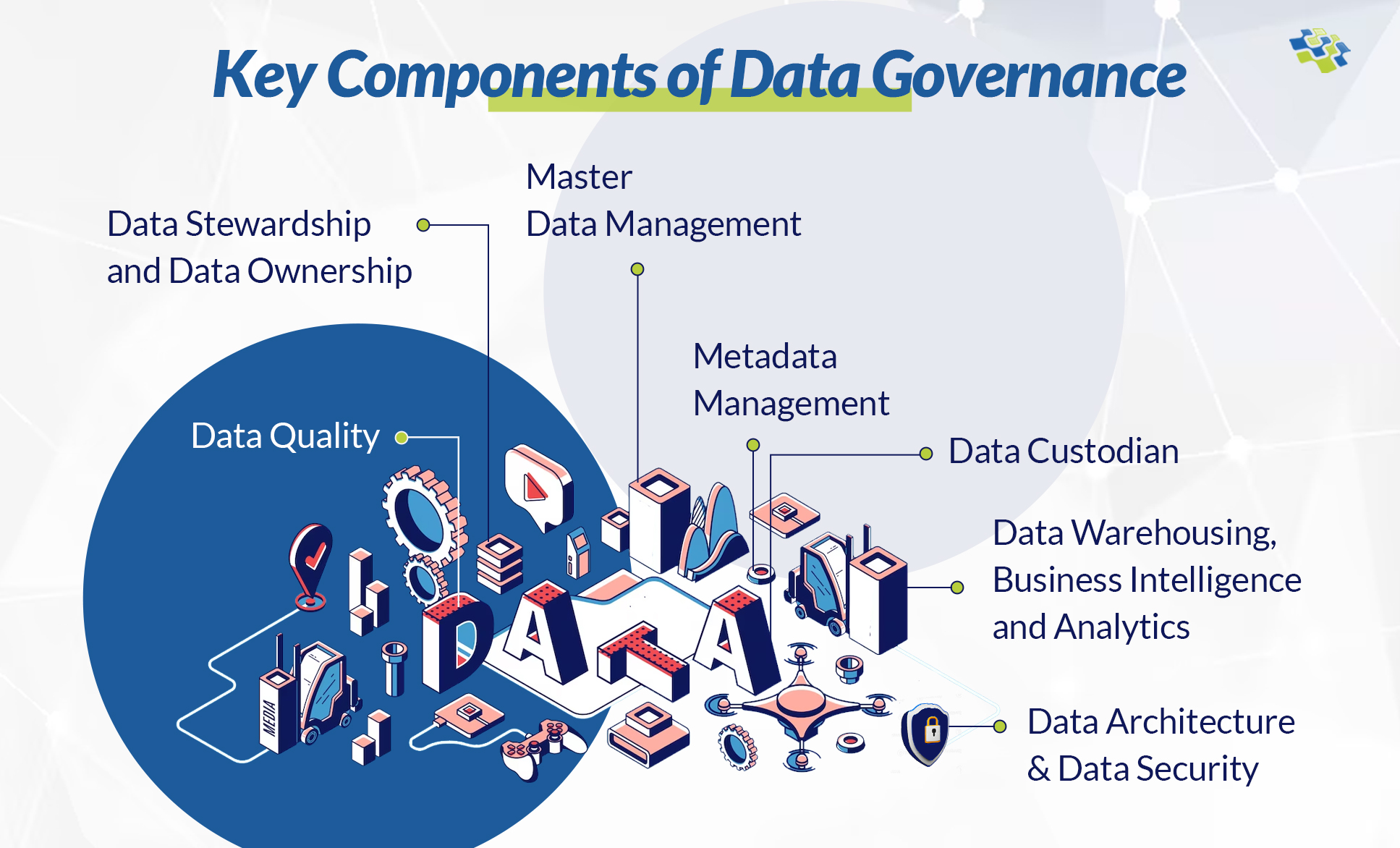
Data Governance Strategy: A Must Have for Every Organizations
Data acts as the linchpin, connecting these diverse technologies. It’s not just the new oil; it’s the lifeblood of the modern business ecosystem. As businesses adapt, every digital interaction generates data, fueling digital transformation.
Stay In the Know
Get Latest updates and industry insights every month.
 1. Digital Twins to Speed Up Clinical Research
1. Digital Twins to Speed Up Clinical Research